The Journey of Donated Blood: From Collection to Patient Care

Meta Title The Complete Process of Blood Donation, Storage, and Transfusion
Meta Description : Learn how blood is collected, stored, classified, and transfused safely. Understand donor precautions, storage life, separation of components, and possible reactions during transfusion.
Focus Keyphrase : Blood donation process and transfusion
Tags: Blood Donation, Blood Bank, Transfusion Medicine, Healthcare, Medical Education
Category: Health & Medicine
Introduction
Blood donation is one of the most vital acts of compassion, saving millions of lives each year. But what happens after blood is collected from a donor? The journey of blood—from collection, storage, classification, separation of components, to transfusion—is a highly regulated process ensuring safety for both donor and recipient.
Collection of Blood from Donors
– Eligibility: Donors must be healthy, aged 18–65, and weigh at least 50 kg. Hemoglobin levels are checked before donation.
– Volume Collected: Typically, 350–450 ml of whole blood is collected in one session. This amount is safe and does not affect the donor’s health.
– Precautions for Donors:
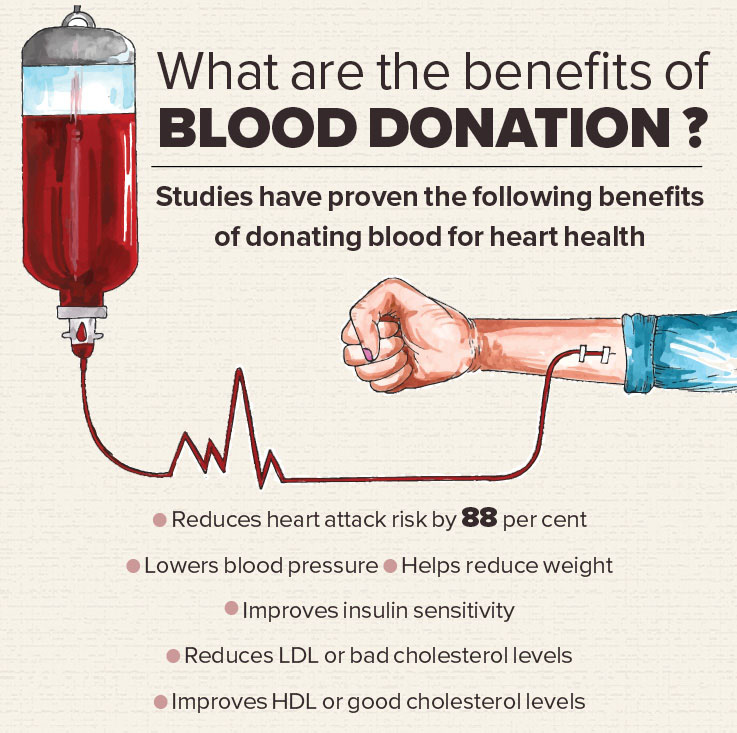
Benefits of blood donation
– Donors are advised to rest before and after donation.
– They should avoid alcohol, smoking, or heavy exercise on the day of donation.
– Hydration and a light meal are recommended before donating.
– Post-donation, donors are observed for 15–20 minutes to prevent dizziness or fainting.
Storage and Transportation to Blood Bank
Once collected, blood is stored in sterile, anticoagulant-treated bags.
– Transportation: Blood is transported in temperature-controlled containers (2–10°C) to ensure viability.
Internal link learn from similar articles
– Documentation: Each unit is labeled with donor details, collection date, and unique identification codes for traceability.
MOHFW guidelines on blood donation
Classification of Blood
Blood is classified based on ABO blood group system and Rh factor (positive or negative).
– ABO Groups: A, B, AB, and O.
– Rh Factor: Determines compatibility (Rh+ or Rh–).
– Cross-Matching: Before transfusion, donor blood is tested against recipient blood to prevent incompatibility reactions.
Storage Conditions and Shelf Life
Different blood components have different storage requirements:
| Component | Storage Temp | Shelf Life | Notes |
| Whole Blood | 2–6°C | 35–42 days | Rarely used directly; usually separated |
| Red Blood Cells (RBCs) | 2–6°C | 35–42 days | Main oxygen carriers |
| Platelets | 20–24°C (with agitation) | 5–7 days | Vital for clotting |
| Plasma | –18°C or lower | Up to 1 year | Used for clotting disorders |
| Cryoprecipitate | –18°C or lower | Up to 1 year | Rich in clotting factors |
Separation of Blood Components
Blood is rarely transfused as whole blood. Instead, it is separated into components using centrifugation:
– Red Blood Cells (RBCs): Settled at the bottom, used for anemia or blood loss.
– Platelets: Extracted from the middle layer (buffy coat), used for clotting disorders.
– Plasma: The liquid portion, rich in proteins and clotting factors.
– Serum: Plasma without clotting factors, used for diagnostic tests.
This separation ensures that patients receive only the component they need.
Transfusion into Patients
When blood is transfused: ICMR guidelines on blood donation and more
– Compatibility Testing: Cross-matching ensures donor blood will not react adversely with recipient blood.
– Mixing with Patient Blood: Donor blood integrates seamlessly into the recipient’s circulation, supporting oxygen transport, clotting, or plasma volume depending on the component given.
Possible Reactions During Transfusion
Although rare, transfusion reactions can occur:
– Mild Reactions: Fever, chills, rash, or itching.
– Moderate Reactions: Shortness of breath, chest pain, or rapid heartbeat.
– Severe Reactions (Hemolytic Reaction):
– Back pain, dark urine, low blood pressure.
– Caused by incompatibility between donor and recipient blood.
– Metabolic Reactions:
– Hypocalcemia: Due to citrate in stored blood binding calcium.
– Hyperkalemia: Potassium leakage from stored RBCs.
– Iron Overload: In patients receiving multiple transfusions.
Immediate medical intervention is required if any reaction occurs.
Conclusion
The journey of blood donation is a remarkable example of science and humanity working together. From careful donor selection and safe collection to meticulous storage, classification, and transfusion, every step is designed to protect lives. Understanding this process not only builds trust in the healthcare system but also encourages more people to donate blood—a gift that truly sustains life.
