Genital prolapse in women happens when pelvic organs like the bladder, uterus, or rectum slip down into the vaginal canal due to weakened muscles and tissues. It can cause symptoms like heaviness, bulging, urinary or bowel problems, and discomfort. Treatment ranges from lifestyle changes and pelvic floor exercises to pessaries or surgery depending on severity.
Genital Prolapse in Women: A Complete Guide in Simple Terms
Meta Description
Learn about genital prolapse in women — definition, types (cystocele, rectocele, enterocele, urethrocele, vault prolapse, uterine prolapse, utero-vaginal prolapse), symptoms, causes, diagnosis, prognosis, and treatment explained in simple layman’s language.
Keywords: Genital prolapse, cystocele, rectocele, uterine prolapse, vaginal prolapse, pelvic floor weakness, prolapse treatment, women’s health, pelvic organ prolapse
What is Genital Prolapse?
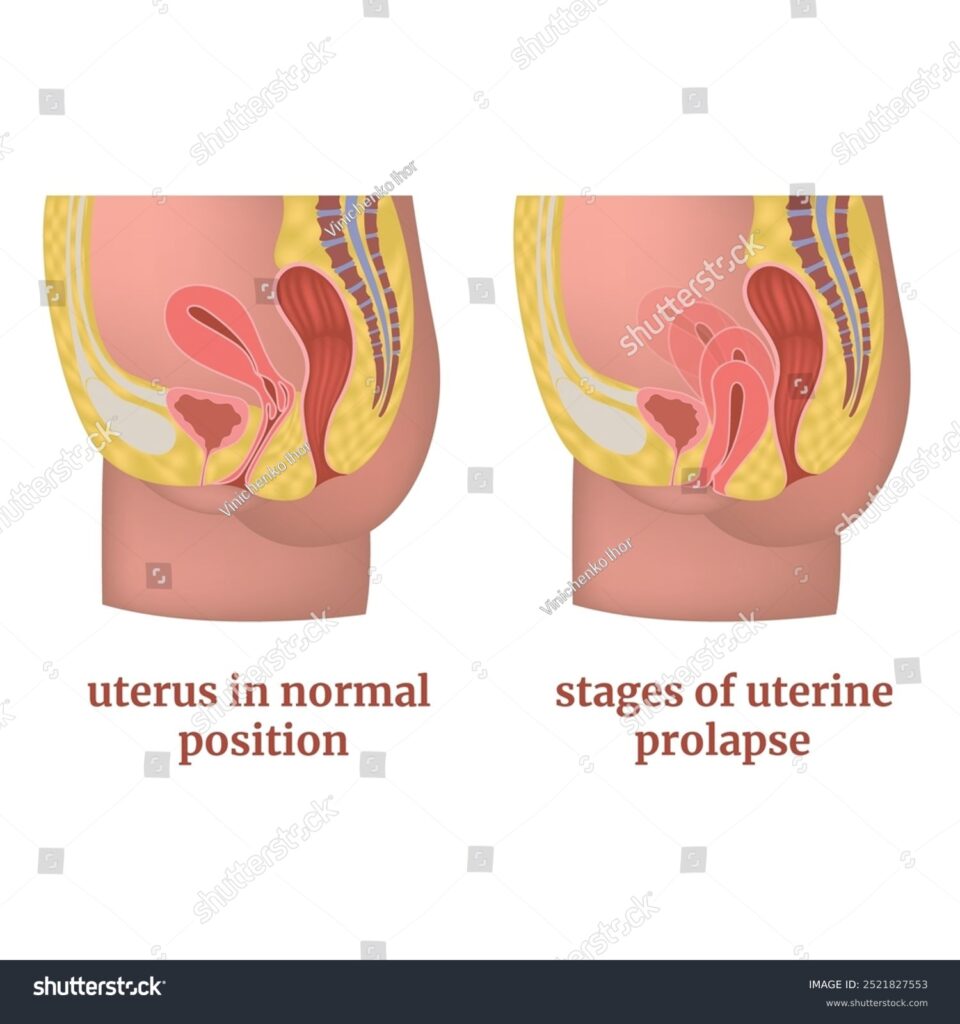
Alt Text Source of Images shuttleck Uterus normal and uterine prolapse
Genital prolapse (also called pelvic organ prolapse) occurs when the muscles and tissues that support a woman’s pelvic organs become weak. As a result, organs like the bladder, uterus, rectum, or vagina slip down from their normal position and bulge into the vaginal canal.
It is more common in women who:
– Have had multiple vaginal deliveries
– Are post-menopausal (due to reduced estrogen)
– Have undergone pelvic surgery
– Experience chronic coughing, constipation, or heavy lifting
Types of Genital Prolapse
1. Cystocele (Bladder Prolapse)
– Definition: The bladder bulges into the front wall of the vagina.
– Symptoms: Frequent urination, leakage, incomplete emptying, heaviness.
– Causes: Weak front vaginal wall, childbirth, aging.
– Treatment: Pelvic floor exercises, pessary, surgery if severe.
2. Rectocele (Rectum Prolapse into Vagina)
– Definition: The rectum bulges into the back wall of the vagina.
– Symptoms: Constipation, difficulty emptying bowels, bulge sensation.
– Causes: Weak back vaginal wall, childbirth trauma.
– Treatment: Fiber diet, stool softeners, surgery if severe.
3. Enterocele (Small Intestine Prolapse)
– Definition: Small intestine pushes into the vaginal canal.
– Symptoms: Pelvic pressure, backache, vaginal bulge.
– Causes: Weak upper vaginal support, hysterectomy.
– Treatment: Surgical repair.
4. Urethrocele (Urethra Prolapse)
– Definition: Urethra slips into the vaginal wall.
– Symptoms: Urinary leakage, difficulty starting urination.
– Causes: Weak pelvic floor, childbirth.
– Treatment: Pelvic floor therapy, surgery.
5. Vault Prolapse (After Hysterectomy)
– Definition: The top of the vagina (vault) drops after uterus removal.
– Symptoms: Vaginal bulge, discomfort during intercourse.
– Causes: Loss of uterine support after hysterectomy.
– Treatment: Surgical suspension of vaginal vault.
6. Uterine Prolapse
– Definition: Uterus descends into the vaginal canal.
– Symptoms: Feeling of something “coming down,” pelvic heaviness, backache.
– Causes: Weak uterine ligaments, childbirth, aging.
– Treatment: Pessary, hysterectomy, or uterine suspension surgery.
7. Vagino-Uterine Prolapse / Utero-Vaginal Prolapse
– Definition: Both uterus and vaginal walls descend together.
– Symptoms: Combined bladder, bowel, and pelvic pressure problems.
– Treatment: Depends on severity — pessary or surgery.
Symptoms of Genital Prolapse
– Vaginal bulge or lump
– Pelvic heaviness or dragging sensation
– Urinary leakage or difficulty urinating
– Constipation or bowel difficulty
– Discomfort during intercourse
– Lower back pain
Causes (Aetiology)
– Childbirth trauma (especially multiple deliveries)
– Menopause (loss of estrogen weakens tissues)
– Chronic straining (constipation, coughing, heavy lifting)
– Pelvic surgery (like hysterectomy)
– Genetic weakness of connective tissue
Diagnosis
Doctors use:
– Pelvic examination (to see bulge)
– Ultrasound or MRI (to check organ position)
– Symptom history (urinary, bowel, sexual issues)
Prognosis
– Mild cases: Often manageable with lifestyle changes and exercises.
– Moderate cases: May need pessary support.
– Severe cases: Surgery usually restores function, though recurrence is possible.
Treatment Options
1. Lifestyle & Prevention
– Avoid heavy lifting
– Treat constipation
– Maintain healthy weight
2. Pelvic Floor Exercises (Kegels)
– Strengthen muscles supporting pelvic organs
3. Pessary Device
– A removable device placed in the vagina to support organs
4. Surgery
– Vaginal or abdominal repair
– Hysterectomy (for uterine prolapse)
– Vault suspension (for vault prolapse)
Conclusion
Genital prolapse is common but treatable. Early recognition and lifestyle changes can prevent worsening. With proper medical care, most women regain comfort and quality of life.
Disclaimer
This blog is for educational purposes only. It is not a substitute for professional medical advice. Please consult a gynecologist for personalized diagnosis and treatment.
Sources:
– Medicover Hospitals – Female Genital Prolapse
– Cleveland Clinic – Vaginal Prolapse
– Verywell Health – Vaginal Prolapse Types & Treatment

Good
Nice
Best
Best luck
Nice 👍