This blog reveals a detailed overview of Oral Submucous Fibrosis (OSMF) — covering anatomy, pathogenesis, clinical progression, inflammatory changes/ulcers, risk from areca nut/spicy foods, modern diagnostics & pathology, treatment, and how government schemes/insurance (in India) help patients (especially the poor). You may wish to consult a specialist (oral & maxillofacial surgeon or oral pathologist) for your particular case.
Alt Text Chewing Gutka ,tamaku (Tobacco chewing) invitation to death
1. Basic anatomy of the oral cavity relevant to OSMF
To understand how OSMF develops you first need to visualise the anatomy of the mouth and related structures (tongue, palate, tonsils, muscles) that get involved.
Anatomical overview
Key structures:
- Hard palate & soft palate (upper plate): The hard palate is the bony roof of the mouth; the soft palate (and uvula) is posterior, muscular and more flexible.
- Buccal mucosa / labial mucosa / submucosa: The lining of the inner cheeks and lips; under these you have lamina propria and submucosal connective tissue.
- Tongue: A highly muscular organ (intrinsic and extrinsic muscles) that occupies the floor of the mouth; covered by mucosa and has rich vascular/lymphatic supply.
- Tonsils (particularly palatine tonsils, and sometimes involvement of the oropharynx): Lymphoid tissue located in the fauces (between the palatal arches) that can be adjacent to or involved in pathologic processes of the mouth and pharynx.
- Muscles of mastication & of the oral floor: e.g., masseter, temporalis, medial/lateral pterygoids, mylohyoid, geniohyoid and suprahyoids — these control opening/closing and movement of jaws, tongue, floor of mouth.
- Mucosa → lamina propria → submucosa → muscle/fascia: The mucosal lining overlies connective tissue and then muscle and deeper structures; disease processes in OSMF often affect the sub-mucosal connective tissue (lamina propria, submucosa) and may secondarily involve muscle.
Why this anatomy matters in OSMF
In OSMF the disease process begins in the mucosa/submucosa (especially the lamina propria) and leads to fibrosis (scarring) of that layer and sometimes deeper tissues. This fibrosis reduces elasticity. Because many of the structures (palate, buccal mucosa, floor of mouth, tongue) are mobile and rely on the flexibility of the submucosa and muscle movement, when fibrosis sets in — movement is restricted. Further, the tongue and soft palate, tonsil region may become affected because they share mucosal surfaces and are within the same functional oral cavity space.
2. What is OSMF, and how does it start & progress (gradual stiffening, reduced opening)

Alt Text :OSMF how does it start & progress (gradual stiffening, reduced opening
Definition & basic facts
- OSMF is described as a chronic, insidious disease of the oral cavity and sometimes the pharynx, characterised by juxta-epithelial inflammatory reaction and subsequent fibroelastic changes of the lamina propria (connective tissue just beneath the mucosa), with resultant epithelial atrophy and progressive stiffness of the oral mucosa.
- It is also recognised as a potentially malignant disorder (i.e., premalignant) of the oral cavity — meaning it has a risk of transforming into oral cancer.
- The key point: while the mucosa is first involved (with inflammatory changes) the hallmark is progressive fibrosis of submucosal tissues leading to reduced mouth opening (trismus), loss of flexibility, stiff lips/cheeks, tongue and ultimately functional impairment.
MOHFW guidelines Read more
How it starts & progression
- Early stage: Patients may experience burning sensation (especially on eating spicy food), blanching of oral mucosa, occasional ulceration, stiffness in cheeks/soft palate. Fibrous bands (palpable) begin to appear underneath mucosa.
- Progression: As more collagen is deposited in the submucosa, the mucosal layer becomes less elastic, fibrous bands increase, mucosa may appear blanched or marble-white in places. The tongue, soft palate, buccal mucosa, lips get progressively involved. Because the submucosa and muscle layers lose elasticity, the ability of the jaws to open fully reduces. The inter-incisal mouth opening distance decreases (a measure of trismus).
- Advanced stage: Severe restriction of mouth opening, stiff mucosa, shrunken uvula/soft palate may occur, tongue mobility severely compromised, adjacent muscles may undergo degenerative changes, eating/swallowing becomes difficult, speech and oral hygiene get impacted. The risk of malignant transformation is higher.
Why the mouth muscles & opening reduce
- The fibrotic changes are not just in the superficial mucosa but involve deeper connective tissue and sometimes muscle degeneration (atrophy and replacement by fibrous tissue).
- As the connective tissue becomes stiff and less extensible, structures like the buccal mucosa and the floor of mouth cannot stretch when the jaw opens. Also, the fibrous bands can act like cords restricting movement.
- The musculature (e.g., pterygoids, masseter, tongue muscles) if secondarily involved cannot contract/relax normally because of surrounding fibrosis and reduced mobility of their attachments.
- Over time, repeated injury and insufficient repair (due to chronic insult) lead to scar‐like tissue, decreased muscle mass, and reduced mouth opening (trismus). Some authors describe it as an “over-healing wound” scenario.
Thus OSMF gradually moves from burning/ulceration and mucosal changes → fibrous bands → stiff mucosa/submucosa → muscle involvement → reduced mouth opening.
3. How the upper plate (palate), tongue, tonsils get inflamed/ulcers in OSMF
Upper plate (hard/soft palate) involvement
- The palate (especially soft palate) is a common site for OSMF changes because the mucosa here is subject to chronic irritants (chewing substances may spread posteriorly) and the submucosa has fibroblastic tissue that can be triggered into fibrosis.
- Initially there may be blanching of the mucosa (whitening) and early fibrous band formation in the lamina propria beneath the mucosa of the palate. The palate may lose its flexibility; the soft palate may not move well during speech/swallowing.
- As fibrosis deepens, the upper plate surfaces (hard/soft palate) become rigid; the uvula may shrink (“bud-like shrunken uvula”) and movement of soft palate/velopharyngeal closure during speech/swallow is compromised.
Tongue involvement
- The tongue may show restricted protrusion or lateral movement because the surrounding mucosa and submucosa (floor of mouth, lateral borders) become fibrotic.
- Fibrous bands may involve muscles of the tongue or its attachments, making it less mobile; this contributes to difficulty in speaking, swallowing, and oral hygiene.
- Ulceration may occur on the tongue’s dorsal or lateral surfaces due to friction, irritation from sharp teeth, or chronic injury in presence of restricted mobility and compromised mucosa. The mucosa may appear atrophic and red or ulcerated because it cannot respond normally to injury.
Tonsils / oropharyngeal involvement
- Although the primary focus is the oral cavity, OSMF can extend posteriorly to involve oropharyngeal mucosa, including the tonsillar region and pharynx, because the same chronic irritant exposures (areca nut, gutkha) affect entire mouth and throat lining.
- The mucosa of the tonsillar region may undergo juxta-epithelial inflammation, fibrous band formation and such changes. As a result, tonsils may feel firm, restricted movement of soft palate may impair speech/swallow, and the throat may feel stiff.
- Ulcers may develop in these regions due to chronic smearing of irritants, burns from spicy/hot food/liquid, or mechanical trauma (e.g., from fibrotic mucosa).
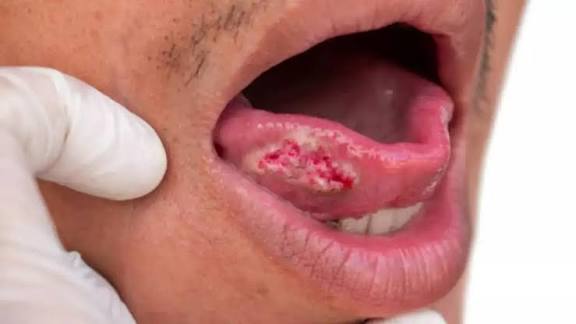
Ulcers & reddish mucosal changes
- Early in OSMF you may see burning sensation when eating hot/spicy food (because the mucosa is sensitised and the submucosa is inflamed).
- Ulcers (shallow erosions) may appear on mucosal surfaces because the fibrotic tissue has reduced vascularity and healing capacity. The mucosa is thin/atrophic and less able to tolerate trauma.
- Reddish signs (erythema) may be seen in the background of mucosal change (blanching, marble-appearance, pale bands) because of underlying inflammatory reaction and microvascular changes. Over time the mucosa may become pale, with visible fibrous bands, or appear marbled (alternating pale and red).
Why spicy food makes it worse
- Spicy foods (chilli, hot sauces) and irritants cause burning sensation, especially when mucosa is already compromised (thin atrophic epithelium, underlying inflammation, reduced protective function). The burning triggers sensory nerves, causes discomfort, and may aggravate the inflammatory reaction.
- Additionally, hot/spicy food may irritate mucosa already damaged by fibrotic change, triggering ulceration or exacerbating existing ulcers. The compromised tissue has less resilience.
- Chronic irritation (from spicy/hot/acidic food) promotes further inflammation → triggers fibroblastic activity → more collagen deposition → worsening fibrosis. So while they don’t cause OSMF, they worsen symptoms and accelerate progression.
4. Why chewing areca nut (“supari”), arecoline (and commercial preparations) leads to a precancerous stage
Role of areca nut / arecoline
- One of the strongest etiologic associations in OSMF is chronic chewing of Areca nut and its commercial preparations (gutkha, pan masala, betel quid with areca nut) — especially in South Asia.
- Areca nut contains arecoline (an alkaloid) and other compounds which stimulate fibroblasts to produce more collagen, inhibit collagen degradation (i.e., decreased activity of collagenases), generate reactive oxygen species (ROS) and cause chronic inflammatory changes in submucosa.
- The fibrotic process is thus triggered by a combination of:
- Persistent irritant exposure (chewing habit)
- Juxta-epithelial inflammation (increased fibroblasts, inflammatory cells)
- Excess collagen deposition (especially types I and III)
- Decreased collagen breakdown (so the scar tissue accumulates)
- Atrophy of overlying epithelium, stiffening of mucosa, reduced blood supply.
Why precancerous / malignant potential
- OSMF is classified as a potentially malignant disorder because the changes in mucosa and submucosa (especially epithelial atrophy, chronic inflammation, oxidative stress) increase the risk of transformation to oral squamous cell carcinoma (OSCC).
- The chronic injury/inflammation → fibrosis → impaired vascular/immune surveillance → can allow dysplastic epithelial changes to develop.
- The commercial preparations of areca nut often include tobacco, slaked lime, spice — amplifying carcinogenic risk.
- The longer the habit (duration of chewing), higher the cumulative exposure, greater the fibrotic and dysplastic changes. Early cessation reduces risk.
Summary: Mechanism simplified
- Habit (areca nut chewing) → constant mechanical/chemical irritation of oral mucosa.
- Juxta-epithelial inflammatory response triggered.
- Fibroblasts proliferate, deposit collagen; collagen breakdown reduced.
- Submucosa becomes fibrotic, mucosa becomes atrophic.
- As fibrosis progresses, mucosal movement and elasticity reduced → functional impairment (mouth opening, tongue movement).
- Meanwhile epithelial changes under chronic insult lead to dysplasia → possible malignant transformation.
- Spicy/hot foods, tobacco, alcohol act as aggravating co-factors.
So chewing areca nut is the initiating event; the presence of arecoline and other agents drives the fibrotic process; this leads to OSMF, which is precancerous.
5. Modern pathological tests, investigations (biopsy, biomarkers etc) for OSMF
Investigations & pathology
- Clinical diagnosis is often based on history (habit of areca nut chewing) + findings (blanched mucosa, palpable fibrous bands, restricted opening, burning sensation).
- Biopsy (histopathology): To confirm diagnosis, evaluate epithelial dysplasia (if any), assess submucosal fibrosis, muscle degeneration. Histologically one sees juxta-epithelial inflammatory infiltrate, fibroelastic change of the lamina propria, loss of vascularity, hyalinised collagen bands, possibly muscle degeneration.
- Staging / classification: Several classification systems exist (e.g., by inter-incisal opening, functional impairment, fibrous band presence) to guide treatment and prognosis.
- Imaging / adjuncts: Occasionally imaging (MRI/CT) may be used if deeper involvement suspected (e.g., pterygoid muscle infiltration) though not routine.
- Biomarkers / research tests: Studies have looked at biochemical markers (e.g., collagen type I/III expression, matrix metalloproteinases – MMPs, oxidative stress markers) to predict severity or malignant potential, though these are largely research tools not standard in routine practise.
- Mouth opening measurement: Functional test – measure inter-incisal distance (distance between upper and lower front teeth when mouth opened as wide as possible). This is a simple functional indicator of severity.
Practical pathology/biopsy steps
- A small incisional biopsy is taken from affected mucosal area (ideally from the most clinically suspicious area, e.g., fibrous band + adjacent epithelium).
- The pathologist reports on: epithelial thickness/atrophy, presence of dysplasia, submucosal fibroelastic change, muscle involvement, vascularity, inflammatory infiltrate.
- Based on findings + clinical features a decision is made on management and surveillance for malignant transformation.
Why early diagnosis is important
- Because once fibrosis sets in and becomes severe, reversal is difficult – earlier intervention (habit cessation, medical treatment) yields better results.
- Also detecting dysplasia early allows cancer prevention strategies.
6. Treatment of OSMF
Treatment is multimodal: habitual cessation, medical therapy, physiotherapy, surgical intervention in advanced cases.
Habit cessation & lifestyle
- Stop chewing areca nut and gutkha/pan masala immediately — this is the foundational step.
- Avoid smoking, alcohol, and irritants (very spicy/hot foods, very hot beverages) — these aggravate the mucosa and speed progression.
- Good oral hygiene and removal of sharp teeth/edges that can cause trauma to mucosa.
Medical/Non-surgical therapies
- Intralesional injections: Hyaluronidase + corticosteroids into fibrous bands to reduce fibrosis.
- Systemic therapy: Lycopene (antioxidant), pentoxifylline, interferon-gamma (anti-fibrotic effects), other vitamins (A, C, E) and iron supplementation if needed.
- Mouth opening exercises: Using devices (e.g., wooden spatulas, thermoplastic mouth openers) to increase the inter-incisal opening and elasticity of tissues.
- Nutritional support: Many patients may have nutritional deficiencies which exacerbate OSMF. Improving diet helps.
Surgical/Interventional therapy
- In moderate to severe cases (with very restricted mouth opening or when bands prevent opening/eating) surgery may be required: release of fibrous bands, coronoidectomy (if jaw closure compromised by pterygoid fibrosis), grafting (e.g., skin graft/dermal graft) to reconstruct mucosal defects.
- Micro-surgery under general anaesthesia may be indicated in severe trismus.
- Post-operative physiotherapy is critical to maintain mouth opening.
Monitoring & malignant potential
- Regular follow-up (every 3-6 months or as advised) with clinical exam and, if indicated, repeat biopsies to check for dysplasia/early malignancy.
- Educate patient on symptoms of change (persistent ulcer, red/white patch, new fibrous band, pain, swelling) and earlier presentation is better.
Summary of treatment strategy
- Early stage: habit cessation + medical/physiotherapy
- Moderate stage: above + intralesional therapy + intensive mouth exercises
- Advanced stage: above + surgery (band release/graft) + long-term follow-up
7. Government/organisational support in India for OSMF patients (financial aid, insurance)
Key schemes
- Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (PM-JAY) offers health insurance coverage to economically vulnerable families in India. It includes packages for oral & maxillofacial surgery such as “release of fibrous bands & grafting – in (OSMF) treatment under GA” with a defined package cost.
- The National Health Authority (NHA) publishes a “Health Benefit Package” (HBP) list which includes dental/oral-maxillofacial surgery procedures. For instance the HBP-2.1 PDF shows a code SM007A: release of fibrous bands & grafting in OSMF treatment under GA.
- State-level schemes also list packages and have specified reimbursement rates. For example, the Maharashtra Jan Arogya Yojana list shows OSMF band release & grafting under category S20PM1.3 with a package cost of ₹3,000.
What this means for patients
- If a public/empanelled hospital is approved under PM-JAY, a patient from eligible family can receive cashless or subsidised treatment for eligible procedures listed under the scheme.
- For OSMF patients from economically weak backgrounds, this means that if surgery (band release + grafting) is needed, it may be covered by insurance and reduce out-of-pocket expense.
- Private hospitals also sometimes have “cashless treatment” options under such schemes (as mentioned in ej. the “Dental Park” case) for OSMF patients.
Procedure to avail the insurance / scheme
- Eligibility check: The patient must belong to a family eligible under PM-JAY (based on state criteria, SECC list etc).
- Empanelled hospital: Treatment must be in an empanelled hospital (public or private) that is part of the scheme.
- Pre-authorisation: The treating hospital initiates a pre-authorisation request to the insurance scheme/NHA for the planned procedure (e.g., OSMF fibrous band release).
- Documentation: Clinical notes, investigation reports, biopsy/histopathology (if required), photographs, consent forms. For OSMF, the package documents require clinical notes, post-treatment photo, discharge summary etc.
- Cashless settlement: Once approved, the insurance pays the hospital (or reimburses) per the package rate; the patient does not have to pay (or pays minimal).
- Follow-up: The hospital must upload discharge summary and follow-up data to the scheme portal; patient must attend follow-up as per protocol.
Financial & other organisational help
- Many NGOs and charitable trusts also assist patients with OSMF (especially poor patients) for surgery, rehabilitation, prosthetics (in case of post-cancer changes) or support groups.
- Government campaigns for cessation of areca nut/gutkha, awareness drives in high-risk communities, screening programmes (oral visual examination) are being strengthened.
8. Summary & key take-aways for patients
- OSMF is a serious, progressive, and potentially malignant condition of the mouth caused largely by areca nut chewing and aggravated by irritants such as spicy foods.
- Early detection (stop the habit, treat early) offers the best chance of preserving mouth opening, tongue mobility, and oral function.
- Once fibrosis sets in significantly, functional impairment (restricted mouth opening) sets in because mucosa, submucosa and muscles become rigid.
- Treatment is multi-modal: habit cessation, medical therapy, physiotherapy, surgical release of fibrous bands + grafting in advanced cases, and long-term surveillance for malignant change.
- For financially poor patients in India, insurance schemes such as PM-JAY provide a mechanism for cashless or subsidised treatment; the hospital must be empanelled and follow the procedure for pre-authorisation.
- Avoiding the initiating habit (areca nut) is the most important preventive step — community awareness, screening and cessation programmes matter.
- If you have OSMF (or suspect it) you should consult an oral & maxillofacial specialist or oral pathologist early — with biopsy, staging and a treatment plan.
Internal link Read more similar health awareness blog on https://cordcraft.in

Good article
Nice